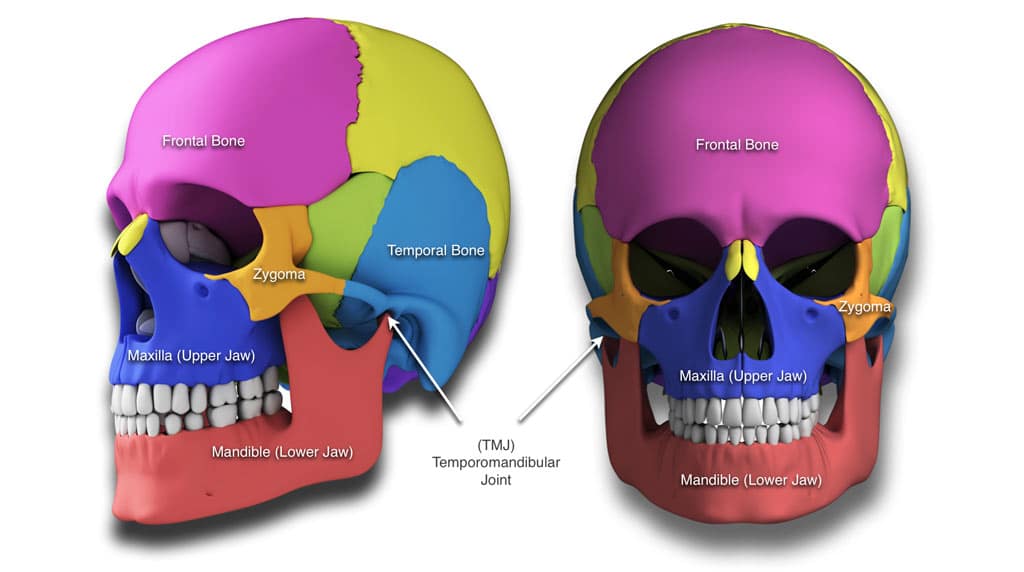
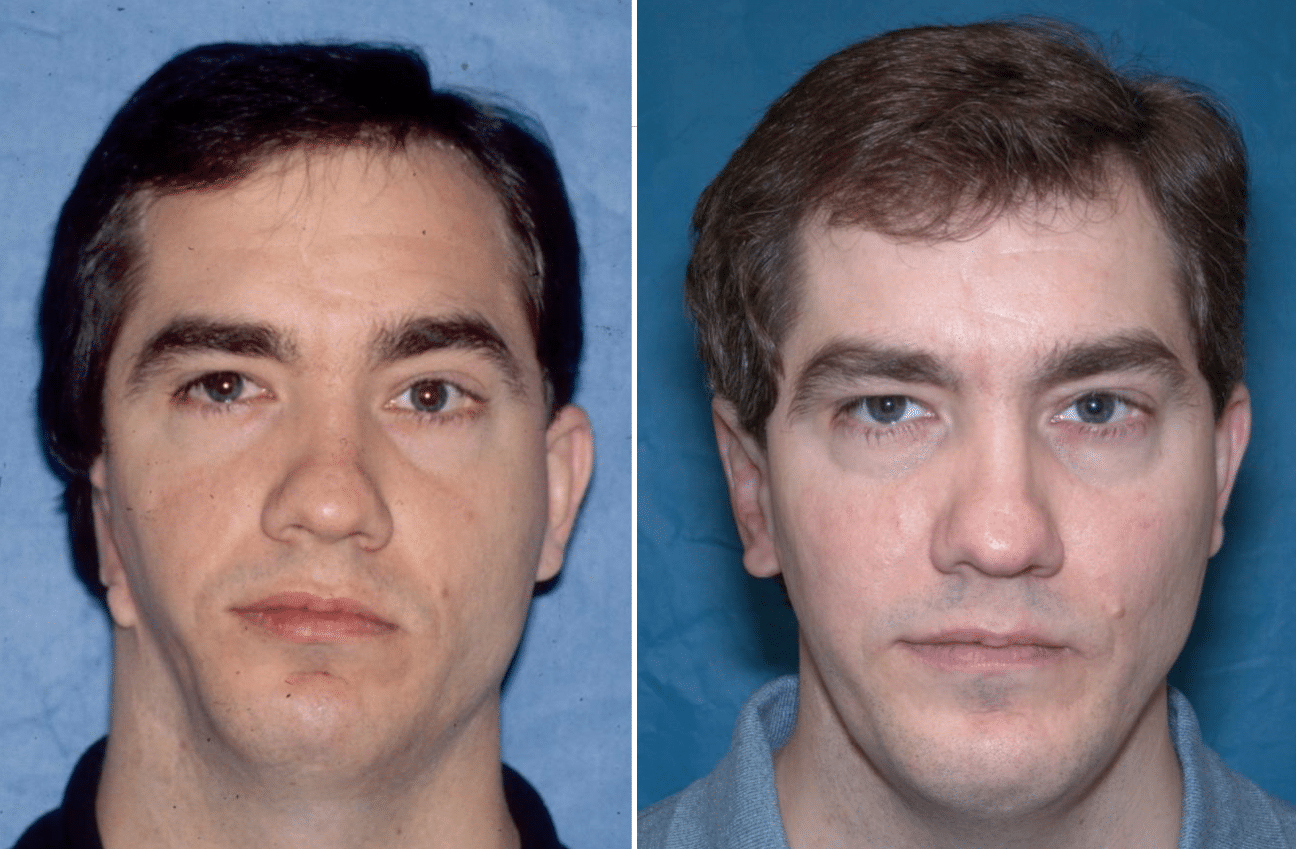
Craniofacial deformities can affect the jaw structures, cheekbones, orbits, nasal complex, TMJ`s, as well as the forehead. Such conditions that Dr. Wolford treats include hemifacial microsomia, Treacher Collins syndrome Crouzon`s syndrome, Apert`s syndrome, cleft lip and palate deformities, as well as many other syndromes.
Dr. Larry Wolford is an internationally renowned oral and maxillofacial surgeon. He is recognized as a leading expert in:
- Orthognathic (jaw correction) surgery
- TMJ surgery
- Airway obstruction
- Sleep apnea treatment
- Cleft lip and palate treatment
- Craniofacial reconstruction surgery
- Nerve repair surgery
Dr. Wolford is responsible for the development of many state-of-the-art procedures currently used in these surgical fields. From diagnosis to treatment and follow-up, he offers unparalleled care for his patients, who are referred from all over the world.
With over 35 years of surgical experience, Dr. Wolford’s expertise is highly sought after to treat the most complex cases, as well as those that have resulted from previously unsuccessful surgeries.
Craniofacial Reconstruction
Craniofacial reconstruction involves surgical procedures that repair abnormalities – craniofacial deformities – of the face and skull usually resulting from birth defects, genetic disorders, traumatic injuries, or cancer. The goal of reconstruction is to restore the jaw, mouth, and sensory organs to functionality, as well as improve physical appearance. Recent advances, which allow for more successful surgeries, have been made in craniofacial reconstruction. These include:
- Surgical plastics that can replace bone grafts
- New techniques for keeping bones in place while healing
- Better understanding of facial soft tissues
- Improved surgical techniques
- Computerized imaging programs that allow doctors to download and analyze data directly from computed tomography (CT) scans or x-rays.
Birth Defects and Genetic Abnormalities
Craniofacial deformities in the growth of the head and facial bones are known as craniofacial anomalies (CFA). These irregularities are present at birth (congenital) and range from mild to severe, often requiring surgery. Congenital disorders that are characterized by CFA include:
Down syndrome: Caused by chromosomal abnormality. Common features are small, rounded ears, flattened nasal bridge, slanted eyes and large protruding tongue.
Crouzon and Apert syndromes: Both involve craniosynotosis that is premature fusing of the fibrous joints in the bones at the top of the skull. Characteristics include sunken-in facial appearance, misshapen head, dental malpositioning, and breathing problems.
Treacher Collins syndrome: Caused by a human chromosome five mutation, abnormalities include small jaw and airway (often causing breathing problems), malformed or missing ears, down slanting eyes, notched lower eyelids, and underdeveloped cheek bones.
Dr. Wolford has been a pioneer in the treatment of many of these syndromes and has developed procedures to provide high quality outcomes for these patients. At your consultation, Dr. Wolford will develop a diagnosis and comprehensive treatment plan to correct your craniofacial deformities issue.
Please contact Dr. Larry Wolford’s office using our online contact form or call 214-828-9115 if you would like to schedule an appointment.